
Key Takeaways
| Topic | Key Fact |
|---|---|
| Market Size | Medical transcription software market valued at $2.55B in 2024, projected to reach $8.41B by 2032 |
| Time Saved | Physicians save 8+ hours weekly — a 70% reduction in charting time — with AI dictation |
| Accuracy | Medical-grade AI speech recognition hits 93–98% accuracy on clinical terminology |
| HIPAA Compliance | Requires a signed BAA, AES-256 encryption, and compliant data handling from the vendor |
| Cost Range | Tools range from $49/month (HealOS) to $400–500/month (DeepScribe) |
| Burnout Link | Over 50% of U.S. physicians report burnout, with EHR documentation as a leading cause |
| Ambient AI | Ambient scribes reduce after-hours documentation by 30% and increase note well-being by 30.7% |
Doctors spend roughly two hours on paperwork for every single hour they spend with a patient. Two hours. That's not a minor inconvenience — it's a systemic failure that drives burnout, documentation errors, and genuinely worse patient outcomes. Voice-to-text for medical professionals has been around since the early '90s, but today's AI dictation tools are a different animal entirely. They actually understand clinical language, format structured notes on their own, and some will just... listen through an entire patient encounter without the clinician saying a single extra word.
This guide covers how dictation software for medical professionals works in 2026, which tools are actually worth your time, what HIPAA compliance really requires (not just the checkbox version), and how to pick the right one for your practice.
What Is Medical Dictation Software, and Why Do Doctors Need It?
Nevertheless, Medical dictation software converts a clinician's spoken words into written text — either in real time or from a recorded encounter. That's the simple version. Hence, It's been around for decades, but today's AI-powered tools do a lot more than basic transcription.
Therefore, Modern doctor dictation software doesn't just capture words. It understands the context of a clinical conversation, automatically formats notes into SOAP or DAP structures, integrates with EHR systems like Epic and Cerner, and in some cases generates a complete clinical note after a patient visit ends — without the physician saying a single extra word. Consequently, Not bad.
Why does it matter so much? The data is pretty blunt:
- Physicians spend approximately 34% of their total work time on documentation
- For every 1 hour of patient care, clinicians log roughly 2 hours of EHR and desk work
- More than 50% of U.S. physicians report burnout, with EHR documentation consistently ranked as a primary driver
- The medical transcription software market was valued at $2.55 billion in 2024 and is projected to reach $8.41 billion by 2032, with a CAGR of 16.3%
The problem isn't that clinicians can't write. It's that the required volume of documentation has just exploded over the years, and typing every note by hand doesn't scale. Furthermore, At all.
That's where speech-to-text for healthcare comes in. A physician can dictate clinical notes in real time, review and sign a note generated from a patient conversation, or use ambient AI to passively capture the entire encounter. Additionally, Each approach cuts time in the EHR — and for high-volume practices, those savings stack up fast.
Here's what separates AI transcription for clinical notes from a regular consumer speech app: medical vocabulary. Hence, General apps hit 70–80% accuracy on clinical terms. Therefore, Purpose-built medical dictation tools reach 95% or above — because they're trained on clinical terminology, drug names, procedural codes, and anatomical language.
Additionally, That gap matters a lot more than it sounds. A transcription error in an email is annoying. In a patient record, it can be a clinical risk.
Nursing staff, therapists, radiologists — really, any role that generates clinical documentation — can get something out of this through allied health applications. It's not just for physicians.
The Documentation Crisis Burning Out Physicians
A physician earning $300,000 annually who saves just 20 minutes per day on documentation is effectively recapturing around $15,000 in annual time value. Multiply that across a hospital system with hundreds of clinicians and the financial case is pretty obvious. But honestly, the human case matters more.
Research published in npj Digital Medicine found that documentation burden is one of the single biggest barriers to scaling AI adoption in clinical settings — but it's also one of the most solvable. That's actually a rare combination.
Consequently, Some specific figures that show how serious this is:
- A rapid review in JMIR AI found that ambient AI scribes saved over 15,700 hours of documentation time across 2.6 million patient visits
- Emory Healthcare saw a 30.7% increase in documentation-related well-being after adopting ambient AI tools, per a 2025 JAMA study
- Physicians using ambient AI scribes spent 20.4% less time on notes per appointment (from 10.3 down to 8.2 minutes average)
- After-hours charting dropped by 30% among clinicians using ambient documentation AI
- Same-day appointment closure improved by 9.3%
The burnout connection is pretty direct. Physicians who finish a full day of patient care and then sit down to two-plus hours of charting burn out faster — it's not complicated. Some are leaving the profession entirely. Others are cutting clinical hours. And the pipeline of new physicians can't keep up with attrition that's partly driven by paperwork.
Nonetheless, Voice to text for doctors isn't a premium upgrade anymore. For many practices, it's a retention tool — full stop.
There's also a quality argument worth making. Fatigued physicians make documentation errors. Notes written at 10pm after a 12-hour shift miss clinical details — it's just what happens. Hence, Ambient AI tools capture more complete information because they're not competing for clinical attention during the visit. And research has shown that ambient scribes actually document more diagnoses per encounter than manual charting. Not fewer. More.
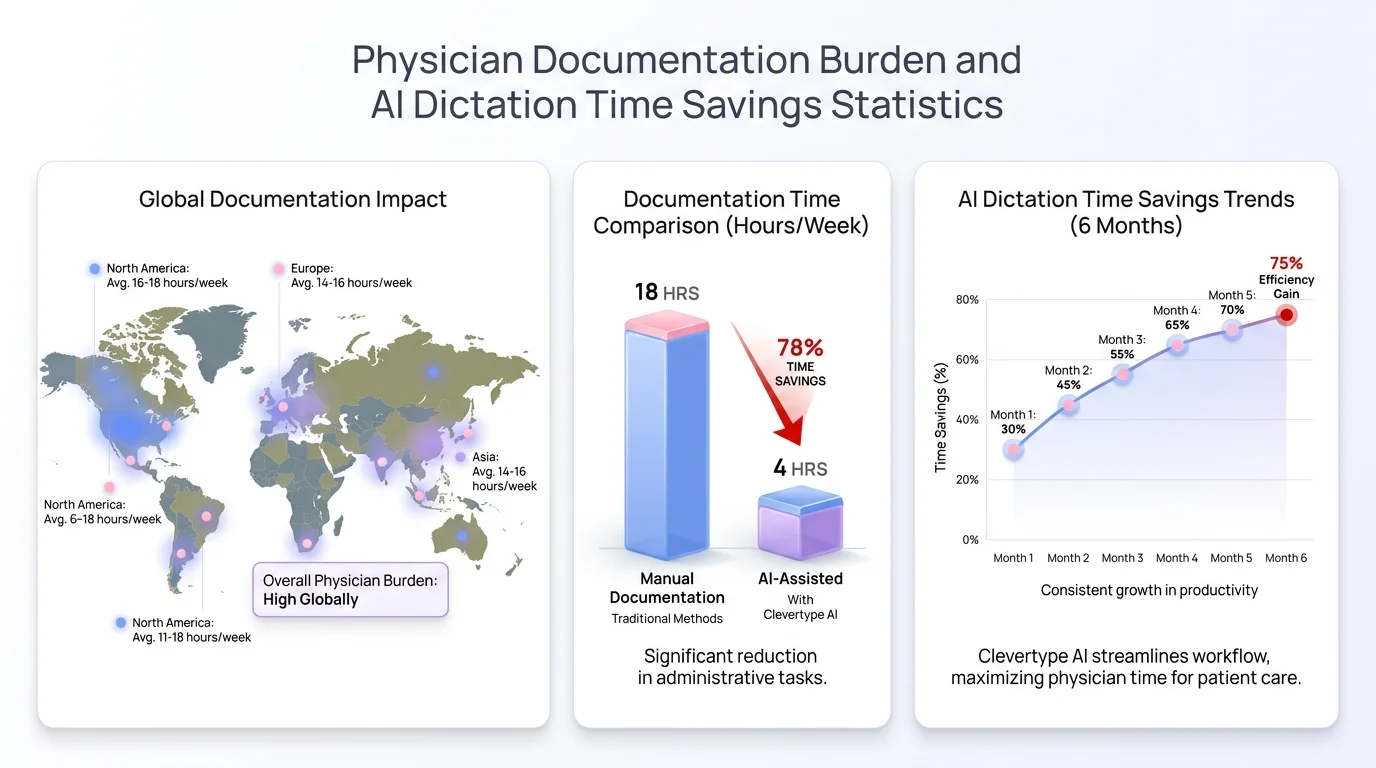
Key statistics on physician documentation burden and the time savings delivered by AI dictation tools in 2026
How AI Speech-to-Text for Healthcare Actually Works
The mechanics behind modern speech to text for healthcare are actually more interesting than they look. At the most basic level, speech recognition converts audio into text using acoustic models and language models. Medical-grade AI goes several layers deeper — and the differences matter:
- Medical vocabulary training — The model is trained on millions of hours of clinical conversations, radiology reports, discharge summaries, and EHR notes. It handles terms like "salpingo-oophorectomy" or "Janeway lesions" without being spelled out.
- Speaker adaptation — Most tools learn an individual physician's voice, accent, and patterns over time, improving accuracy with use.
- Context modeling — The AI knows "BP" in a clinical context means blood pressure, not British Petroleum. It adjusts accordingly.
- Note structuring — Advanced tools don't just transcribe — they output structured SOAP, DAP, or H&P notes automatically, ready for EHR entry.
- Ambient listening — Some tools like Microsoft Dragon Copilot (launched March 2025) and Nuance DAX listen passively to the entire patient encounter and generate a note post-visit, without any active dictation from the clinician.
A systematic review evaluating AI-based speech recognition for clinical documentation found that performance varies quite a bit based on specialty vocabulary, audio environment, and speaker characteristics — but the best systems now approach human-level transcription accuracy in structured clinical settings. That's not marketing copy. Furthermore, That's a real benchmark.
Consequently, The typical ambient workflow looks like this: physician opens the app before walking in, has a normal conversation with the patient, visit ends — and a structured note is already waiting in the EHR, formatted and ready to review. Therefore, Scan it, make a few edits, sign. That's it. Therefore, That's the whole documentation workflow.
Amazon Transcribe Medical gives a good sense of how the underlying API-level technology works. It provides HIPAA-eligible real-time medical transcription with specialty vocabularies for primary care, cardiology, neurology, radiology, urology, and oncology — available as a developer service for practices building custom EHR integrations.
HIPAA Compliant Dictation: What Your Software Must Meet
This part is non-negotiable. Any dictation software for medical professionals that handles patient information in the US must comply with HIPAA — the Health Insurance Portability and Accountability Act.
HIPAA compliant dictation means more than a checkbox on a vendor's marketing page. Furthermore, Here's what to actually check before signing anything:
Business Associate Agreement (BAA)
The vendor must sign a BAA. Additionally, It's a legal document establishing them as a "business associate" who handles protected health information (PHI) on your behalf. No BAA means no HIPAA compliance — regardless of what their website says.
Data Encryption
- AES-256 encryption at rest
- TLS 1.2 or higher in transit
- End-to-end encryption for any audio recordings
Audio Retention Policies
Some platforms store recordings after transcription; others delete them immediately. For maximum patient privacy, platforms that process and delete audio in real time are the better choice. Freed and Wispr Flow explicitly state they don't retain patient recordings at all.
Access Controls and Audit Logs
HIPAA requires audit trails. The software should log who accessed records, when, and what changes were made — and that log needs to be available for compliance review.
Data Residency
For US-based practices, patient data should stay on US servers. Confirm this with the vendor, especially if they're cloud-based.
| Platform | BAA | Encryption | Audio Retention | Certification |
|---|---|---|---|---|
| HealOS | Yes | AES-256 | Not stored | SOC2-aligned |
| Wispr Flow | Yes | AES-256 | Not stored | SOC2 Type II, ISO 27001 |
| Vero | Yes | AES-256 end-to-end | Encrypted storage | HIPAA, PIPEDA |
| Freed | Yes | Industry standard | Not stored | HIPAA |
| Scribeberry | Yes | In transit + at rest | Encrypted | SOC2 Type 2, HIPAA |
| Dragon Copilot | Yes | Enterprise-grade | Configurable | HIPAA, HITRUST |
The BAA is step one. Always. Consequently, Get it confirmed before starting any trial with real patient data.
Additionally, One thing a lot of clinicians miss: HIPAA compliance covers how you use the software, not just the software itself. Running a fully compliant platform on a shared, unlocked device in a waiting room still creates real risk. The vendor's certification doesn't cover your internal workflows — that part's on you.
Best Dictation Software for Medical Professionals in 2026
The medical dictation app market has grown a lot in the last couple years — and the options have gotten genuinely better. Here's a practical breakdown of what's actually getting used in clinical settings right now.
1. Microsoft Dragon Copilot
Furthermore, Dragon Copilot launched in March 2025, merging Dragon Medical One's voice dictation with DAX's ambient listening capability. It's the most feature-rich option out there right now and integrates deeply with Epic and Cerner. Enterprise pricing — this one's for large health systems and hospital groups, not solo practitioners.
2. Nuance DAX / DAX Copilot
Microsoft's ambient AI documentation platform, used at large health systems including Emory Healthcare and Northwestern Medicine. Documented to reduce after-hours charting by up to 30% in clinical research. The strongest option for hospitals and large multispecialty groups — if you can get it approved.
3. HealOS (formerly ScribeHealth AI)
Consequently, At $49/month, HealOS is the most accessible serious medical dictation app for independent practitioners. Nonetheless, It claims 98% accuracy on general medical terms and 95% on specialty terminology. For cost-conscious practices that need real EHR integration without enterprise pricing — this is probably your starting point.
4. DeepScribe
Nevertheless, A fully automated AI medical scribe built for high-volume specialty practices. Nevertheless, Priced at $400–500/month — yes, that's a lot. Therefore, But it's genuinely comprehensive. Nevertheless, Notes get generated from natural conversations, which makes it a strong fit for practices that want minimal clinician involvement in the note-writing process.
5. Freed
Nevertheless, Freed is all about simplicity. It transcribes patient encounters and generates SOAP notes directly. Consequently, HIPAA compliant, doesn't store recordings. Therefore, Very popular with therapists, psychologists, and primary care physicians who want a low-friction setup and don't need a lot of bells and whistles.
6. Abridge
Furthermore, Used at Kaiser Permanente, where around 65–70% of physicians use some element of the platform — which is a remarkably high adoption rate. Strong EHR integration, some patient-facing transparency features, and what feels like a genuinely careful approach to note generation.
| Tool | Monthly Cost | Best For | EHR Integration |
|---|---|---|---|
| Dragon Copilot | Enterprise | Large health systems | Epic, Cerner |
| Nuance DAX | Enterprise | Hospitals, large groups | Epic, Cerner |
| HealOS | $49 | Independent/small practices | Multiple EHRs |
| DeepScribe | $400–500 | High-volume specialty | Epic, Athena |
| Freed | $99 | Solo practitioners | Copy-paste + integrations |
| Abridge | Enterprise | Health systems | Epic |
Additionally, For solo practitioners and small clinics, tools in the $49–99/month range honestly deliver 80–90% of the value of enterprise systems at a fraction of the cost. Consequently, The ROI math works fast — at $99/month, if you're saving 5+ hours of documentation time weekly, you're ahead before the end of month one.
Dragon Medical One vs Modern AI Dictation Alternatives
Dragon Medical One has been the dominant doctor dictation software for over a decade. Still holds a significant share of the enterprise market. But the gap between it and newer AI-native tools has narrowed considerably — more than most people realize.
Dragon Medical One charges roughly $79–99/month per user and delivers proven voice dictation with deep EHR integration. It's reliable, well-supported, and familiar to physicians who've used Dragon products for years. For trained users, it hits near 99% accuracy and handles specialty vocabulary really well.
The main limitation: Dragon Medical One is an active dictation tool. Moreover, The physician speaks the note. Additionally, There's no ambient mode. For workflows where the clinician is comfortable dictating structured notes, that's fine. Therefore, But if you want to just talk to your patient and have a note appear automatically? Therefore, It's not the right fit.
Consequently, The newer generation of Dragon Medical alternatives splits into two main categories:
Active Dictation Tools (similar model to Dragon Medical One)
- HealOS — $49/month, cloud-based, no hardware required
- VoiceboxMD — Streamlined, cloud-based, targeting independent practitioners
- Tali — AI-enhanced dictation with EHR-native commands
Ambient AI Scribes (conversation-based, no active dictation)
- Nuance DAX / Dragon Copilot — Listens during encounters, generates note after visit
- DeepScribe — Fully automated note generation from natural conversation
- Abridge — Ambient with patient transparency features
The core question for any practice: do your physicians want to dictate, or do they want the AI to listen?
Hence, For radiology, pathology, or any specialty where notes follow rigid template-driven structures, active dictation is often preferred. For primary care, pediatrics, psychiatry, or geriatrics — where conversations are unpredictable and wide-ranging — ambient AI tends to deliver bigger time savings.
Therefore, A 2025 study on ambient clinical intelligence found that these tools "significantly reduced provider documentation burden, frustration and burnout" compared to traditional dictation methods. The same study showed measurable improvements in same-day note completion and after-hours work reduction. Hard to argue with that.
Dragon Medical One is still excellent for what it does. But the field has moved fast. Practices that haven't revisited their dictation software options in the last two years may be missing some real upgrades.
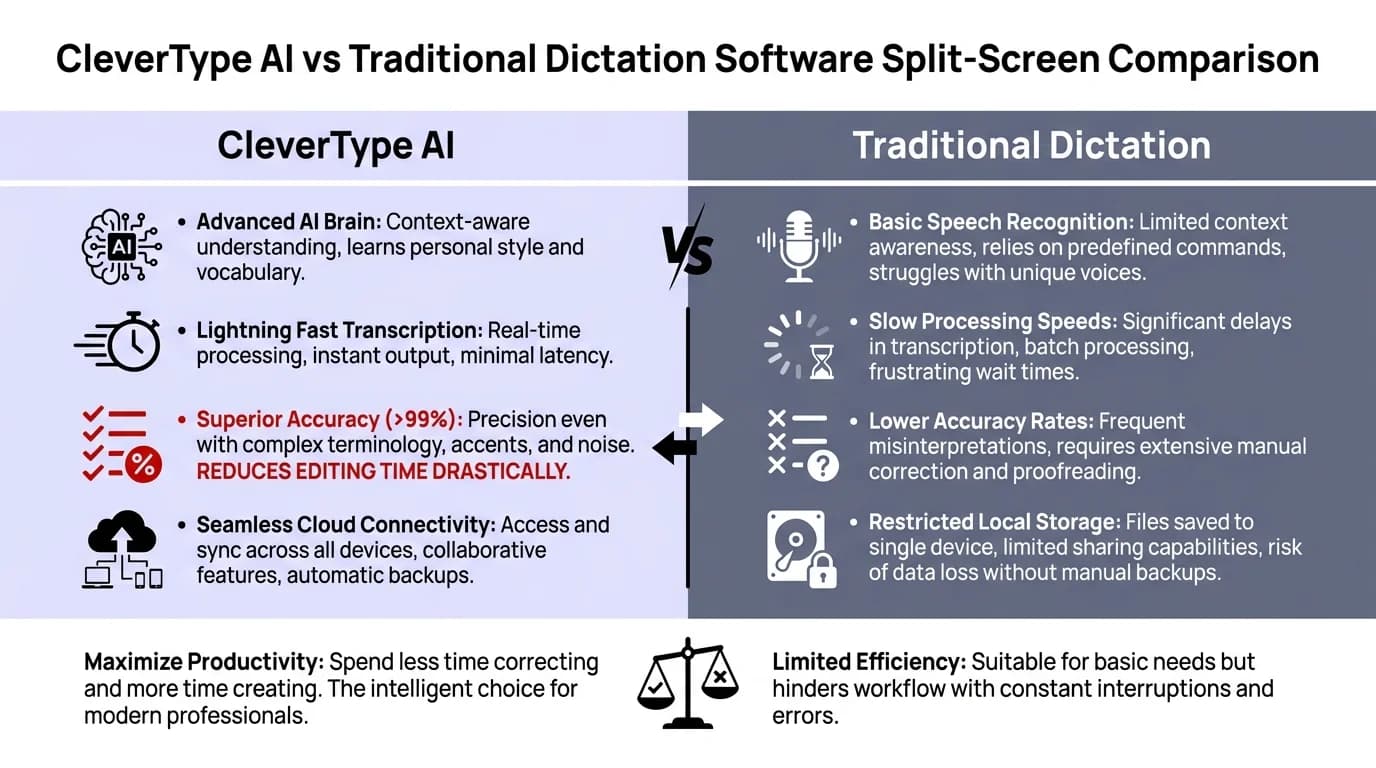
CleverType AI vs traditional dictation software: how modern AI keyboards complement medical dictation workflows for mobile and out-of-EHR documentation
What the Accuracy Numbers Mean for Clinical Notes
Therefore, Accuracy in AI transcription for clinical notes is measured differently than in consumer apps — and honestly, the stakes are different too.
A systematic review of AI-based speech recognition for clinical documentation published in PMC found that performance varies quite a bit depending on:
- Specialty vocabulary depth — General medical terms vs subspecialty nomenclature
- Speaker characteristics — Accent, speech pace, and clarity all affect output
- Audio environment — Background noise in busy clinical settings degrades performance
- Speaker adaptation — Systems that learn a specific clinician's voice over time consistently outperform generic models
| System Type | Accuracy on Medical Terms | Accuracy on General Speech |
|---|---|---|
| Consumer STT (e.g. Siri, Google) | 70–80% | 90–95% |
| Medical-grade STT | 93–95% | 95–98% |
| HealOS (self-reported) | 98% general / 95% specialty | — |
| Speechmatics medical (benchmark) | 93% | 96% |
What does 80% vs 95% actually mean for a 500-word clinical note? Furthermore, Roughly 100 errors versus 25. Some are trivial. Therefore, Some — a misheard drug name, wrong dosage, missed allergy — are not trivial at all.
That's why all serious medical dictation apps include a physician review step. Additionally, The AI generates the draft; the clinician reviews, edits, and signs. The review is usually fast — accuracy is high enough that you're mostly scanning, not rewriting. But physician sign-off is non-negotiable.
There's another side to the accuracy story: what the AI captures that manual charting misses. A 2025 cohort study on Nuance DAX found that using ambient AI increased documented diagnoses per encounter from 3.0 to 4.1. A 37% increase in diagnostic documentation — not because the clinician found more diagnoses, but because the AI captured clinical details that were discussed verbally but would've been left out of a rushed typed note.
Ambient AI doesn't just match manual documentation. In fatigued, high-volume settings, it often exceeds it. Nevertheless, AI doesn't get tired.
How to Choose the Right Doctor Dictation Software for Your Practice
With this many options, picking one can feel overwhelming. It doesn't need to be. Here's a practical framework that actually helps.
Step 1: Identify your primary workflow
Nonetheless, Are you more comfortable actively dictating a structured note, or would you rather the AI just listen during the encounter and generate the note afterward? Both work well — they suit different people and specialties. The honest answer: try both if you can before committing to either.
Step 2: Check EHR compatibility
Nonetheless, Not every tool integrates with every EHR. Epic has the most native integrations; Cerner and Athenahealth follow closely. Furthermore, Some tools use a copy-paste approach when direct integration isn't available — workable, but it adds friction. Nonetheless, Confirm integration depth before signing up.
Step 3: Verify HIPAA compliance properly
Always ask for a BAA before any trial with real patient data. Confirm AES-256 encryption, audio retention policies, and data residency. Don't take "HIPAA compliant" at face value — ask for the documentation.
Step 4: Trial with your actual patient population
Most platforms offer 7–30 day free trials. Test with your real case mix, not demo scenarios. Have multiple clinicians use it if you can — voice and vocabulary vary a lot, and one person's experience won't be universal.
Step 5: Calculate the ROI
Nevertheless, If a physician saves 20 minutes daily at a $300k salary, that's roughly $15,000 in recaptured annual time value — per physician. Consequently, Even a $99/month tool pays for itself inside a week. For practices with 5+ physicians, the numbers stack fast.
Step 6: Evaluate specialty-specific vocabulary
Moreover, Some tools have stronger training data for primary care; others for oncology, psychiatry, or radiology. Consequently, Ask vendors specifically about accuracy for your specialty and test with your real terminology during any trial.
For clinicians who also handle typed documentation on mobile — finishing charts from their phone, responding to patient portal messages, or secure messaging outside the EHR — an AI keyboard like CleverType works well alongside dictation tools. It handles context-aware suggestions, grammar correction, and fast mobile typing with a privacy-first design — useful for the parts of clinical communication that happen outside the EHR workflow.
Nevertheless, Bottom line: the best dictation software isn't always the most expensive. Nonetheless, HealOS at $49/month delivers genuinely solid results for solo practitioners and small clinics. Hospital systems benefit most from enterprise-grade ambient tools with deep EHR integration. Match the tool to your actual workflow — not the marketing pitch.
Frequently Asked Questions
Is voice-to-text for medical professionals HIPAA compliant?
Therefore, It depends entirely on the software. HIPAA compliant dictation requires the vendor to sign a Business Associate Agreement (BAA), implement AES-256 encryption, maintain audit logs, and follow compliant data handling practices. All the major medical dictation platforms — HealOS, Freed, Dragon Medical One, DeepScribe, Abridge — offer BAAs and HIPAA-compliant architectures. General consumer voice apps like Siri or Google Assistant are not HIPAA compliant and should never be used for patient documentation. Furthermore, Full stop.
What is the best Dragon Medical alternative in 2026?
Moreover, The best Dragon Medical alternative depends on your workflow. For ambient AI documentation where no active dictation is required, Nuance DAX or Dragon Copilot are the strongest options. For independent practitioners who want cost-effective active dictation, HealOS at $49/month is a direct, capable alternative. For fully automated note generation from natural patient conversations, DeepScribe and Abridge are your best bets.
How accurate is AI transcription for clinical notes?
Medical-grade AI speech recognition hits 93–98% accuracy on clinical terminology, compared to 70–80% for general consumer speech apps. It also gets better over time as the system adapts to your voice and patterns. All tools require physician review and sign-off on generated notes — the review is quick, but you always need eyes on it before anything gets finalized.
Can AI dictation software integrate with Epic and Cerner?
Hence, Yes. Nevertheless, Dragon Medical One, Nuance DAX, Dragon Copilot, Abridge, and DeepScribe all offer direct Epic and Cerner integration. Nonetheless, HealOS supports multiple EHRs including Epic and Athenahealth. Some smaller tools fall back to a copy-paste workflow if direct API integration isn't available for a specific EHR — worth checking compatibility before you commit.
How much time do doctors save with medical dictation software?
Research shows physicians save an average of 8+ hours per week with AI medical dictation — a roughly 70% reduction in charting time. Nevertheless, Ambient AI scribes reduce note time per appointment by about 20%, and after-hours documentation drops by approximately 30%. For a physician spending 2–3 hours nightly on charting, that's 45–90 minutes back per day.
What is ambient AI documentation?
Ambient AI documentation is software that passively listens to a patient-clinician encounter and automatically generates a structured clinical note when the visit ends. The clinician doesn't dictate or talk to the software directly — they just have a normal conversation with the patient. Tools using this approach include Nuance DAX, Dragon Copilot, Abridge, and DeepScribe. Furthermore, It's increasingly the preferred model for primary care and outpatient settings.
Does dictation software work for specialist terminology?
Generally yes, with variation by specialty. HealOS reports 98% accuracy on general medical terms and 95% on specialty terminology. Systems with subspecialty training corpora — oncology, cardiology, radiology — perform better in those fields than general models. Consequently, The best way to assess fit for a specific specialty is to trial the software with real cases during the free trial period.
Ready to Type Smarter?
Nonetheless, Upgrade your typing with CleverType AI Keyboard. Fix grammar instantly, change your tone, receive smart AI replies, and type confidently while keeping your privacy.
Download CleverType FreeAvailable on Android • 100+ Languages • Privacy-First
Share this article:
Sources
- The impact of using AI-powered voice-to-text technology for clinical documentation: a systematic review (PMC)
- Evaluating AI-based speech recognition for clinical documentation: a systematic review (PMC)
- Barriers and opportunities of scaling ambient AI scribes — npj Digital Medicine
- Real-world evidence synthesis of digital scribes using ambient AI — JMIR AI
- The impact of Nuance DAX ambient listening AI documentation: cohort study (PMC)
- Deploying ambient clinical intelligence to improve care: Nuance DAX study (ScienceDirect)
- Microsoft Dragon Copilot launch announcement — Microsoft News
- Amazon Transcribe Medical — AWS